Scoliosis Cobb angle is a diagnostic tool that is utilized to determine and measure the exact degree of side-to-side spinal curvature using an x-ray film. The technique was developed by renowned orthopedic surgeon and Yale medical school graduate Dr. John Cobb. Dr. Cobb was an innovator in the scoliosis diagnosis and treatment sector of orthopedics and was famous for teaching how the majority of scoliosis patients did not need surgical treatment, which was unfortunately commonly over-utilized at the time.
The Cobb angle survives long after Dr. Cobb has passed away. His technique is still used to measure scoliotic degree today, but has also been implemented to measure various other changes in spinal curvature, including kyphosis and changes in spinal symmetry after traumatic fracture of vertebral bones.
This essay details the history and applications of the famous Cobb angle measuring technique for scoliosis evaluation. We will explain why despite its simplicity, the technique is still a valuable tool in any diagnostician’s arsenal 70 years after it was created.
What is the Scoliosis Cobb Angle?
The Cobb angle of measurement is a simple way of determining the angle or angles of a scoliosis curvature in the human vertebral column. Scoliosis involves atypical curvature on the coronal plane of the spine, best represented by a side-to-side swerve when viewed from the direct anterior or posterior view. Scoliosis can demonstrate a single curvature, called a C curve, or might be multiply curved, called an S curve. Each of the scoliotic types will have its own unique degree of curvature and these measurements can be determined using the Cobb angle system.
The Cobb angle is taught to all physicians and chiropractors, but it only regularly used by care providers who actually manage spinal issues, such as kyphosis, vertebral fracture and scoliosis. The technique is based on simple mathematical principles and is considered highly accurate when performed by an expert using a clear radiological study.
Traditionally, the angle is determined using hard copies of x-ray films, a straightedge and a protractor or compass, but now, most care providers use digital x-ray technology with software that greatly simplifies and increases accuracy of measurement. There are also various computer and smartphone software applications that can measure Cobb angle on any image.
Cobb Angle Evaluation Technique
To begin measuring the angle of scoliosis curvature, the physician will first observe the imaging study and determine the uppermost tilted vertebral bone at the top of the curvature. They will then observe the lowermost tilted vertebrae at the bottom of the curvature. They will note the location of these bones.
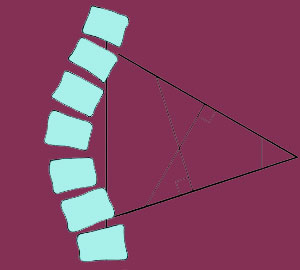
The doctor will then draw a line across the superior endplate of the upper most tilted vertebra, representing the degree of tilt from objective center. They will repeat this step drawing a line across the inferior endplates of the vertebra that is the lowest most tilted from neutral centerline. Where these lines meet forms the Cobb angle.
Since many cases will involve very long lines that will intersect far off the imaging study film, it is easy to simply draw a downward perpendicular line from the uppermost vertebral angle line marker and also draw an upward perpendicular line off the lower most tilted vertebra line marker. Where these 2 lines intersect will also measure the Cobb angle accurately.
For S curvatures, the process is repeated for each aspect of the curvature individually.
Various forms of computer software perform all these tasks in one step, making diagnosis easy and accurate.
Scoliosis Cobb Angle Summary
The main critique of the Cobb angle is the subjectivity of selecting the most tilted vertebral bones during evaluation. In many cases, different doctors will select different vertebra for measurement, based on subjective observation and perception of tilt. This can create results that are not consistent, sometimes being off from one another by 5 to 10 degrees. Obviously this is a major problem, but can be overcome by physicians taking time to perform a thorough and accurate evaluation of each patient or by simply noting which vertebral bones are used and staying consistent with these markers from test to test to check progression.
Additionally spurring along the endplates of selected vertebra might influence measurement as well. Spurs should be taken into account when drawing the lines across any vertebral endplates in order to achieve the most accurate results.
Computers have made both vertebral selection and measurement much more accurate. In fact, the variation in measurements now is typically less than 1% when performed by different doctors on different computer systems, since specialized software is now readily available to take much of the “educated guesswork” out of the equation and replace it with objective factual evidence.
Scoliosis > Scoliosis Diagnosis > Scoliosis Cobb Angle





