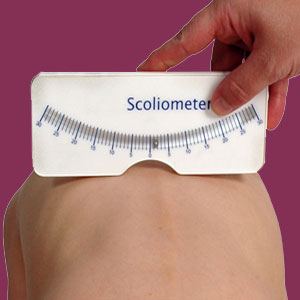
A scoliometer is a simple measuring tool that helps diagnosticians evaluate patients for atypical side-to-side spinal curvature. Although originally designed as a hand-held device that is used as part of a manual and visual examination, there are now high tech versions of scoliosis meters available, ranging from large office-sized devices to ingenious smart phone applications.
This instructional essay explains the proper use of many varieties of scoliosis measuring tools in a clinical setting. We will explain some of the common mistakes associated with the use of these evaluation tools and well as provide advice for clinicians who are trying to achieve the very best and most accurate results possible when identifying and measuring scoliotic formations in the human backbone.
What is a Scoliometer?
This tool is designed to identify potential cases of scoliosis and even measure with approximate accuracy the degree of unusual curvature. The device is often used during diagnostic screening in combination with the Adams Forward Bend Test, although it can be used in cases of diagnosed scoliosis for casual monitoring of the curvature, as well.
The device can help recognize both coronal curvatures, as well as vertebral rotation, so it provides some degree of assessment for a three dimensional plane of scoliotic formation. Scoliosis measuring devices such as this are most often used for thoracic and lumbar scoliosis and are far less useful for diagnosing or evaluating cases of cervical scoliosis or high level cervicothoracic scoliosis.
Types of Scoliosis Diagnostic Tools
The traditional type of device is a simple rectangular shaped object that very much resembles a ruler. It has a curved measuring gauge that extends to both sides of a neutral midline, with a measuring device (needle or ball usually) able to move freely in this gauge. The further the needle or ball moves off center, the greater the degree of curvature that exists at a particular region of the backbone. In the middle of the inferior surface of the device is an anatomically shaped cutout that fits over the spinous processes to guide the evaluator in their assessment of the spine.
However, there are now many varieties of scoliometer available, including fully digital versions, smart phone applications, computerized designs and even virtual versions that utilize lights and tracking software. Technology has increased the applications of scoliosis testing devices, as well as their accuracy by minimizing human error on the part of the diagnostician.
Scoliometer Utilization
The usual technique employed during use of the device is to have the subject bend forward at the waist as far as they can, but not supporting themselves with the hands on their knees or on the floor, as this can influence the reading. The device is placed over the spinous processes near the top of the backbone at an exactly perpendicular angle to the spine. The observer will position themselves to be able to move the device down the spine, while still being able to visualize the gauge to see how the measuring device responds. The diagnostician will take notice of areas where the device peaks in abnormal readings, if any, by noting the vertebral level encountered as the device measures atypical readings.
We recommend the following tips to insure the best outcomes when using this variety of scoliosis measuring device:
Some patients can not bend forward enough to achieve good readings. Try telling them to bend their knees when bending forward or sitting and then bending, as inflexibility is often caused by very tight hamstring muscles.
Screening in obese patients can be challenging. Digital and high technology devices help to overcome the hurdles of these evaluations.
Make sure to visually observe the subject prior to beginning the examination and during the progression of the scoliometer movement, as well. Activity might influence results, so do not be laser-focused on the gauge reading, but instead, try to observe both the device and the subject together.
For best results, screen the subject 2 or 3 times to check the accuracy of readings and minimize the possibility for human error.
Scoliosis > Scoliosis Diagnosis > Scoliometer





